Abstract
Background Diabetes technology can improve glycemic variability and diabetes outcomes, but there are disparities in patient use.
Aims Identify racial, ethnic, and socioeconomic disparities in technology utilization and determine provider-, patient-, and parent-identified barriers.
Methods Technology (continuous glucose monitors (CGM) and pump) usage and demographic data on patients at a large urban pediatric hospital were obtained from a clinical database. Providers (16 attending physicians, five fellow physicians, five nurse practitioners, 13 diabetes educators) completed a survey on diabetes technology prescribing habits. English and Spanish-speaking patients ages 8 to 17 years with diabetes (n=109) and caregivers of pediatric patients with diabetes (n=117) completed surveys that assessed attitudes and perceived benefits/burdens of diabetes technology.
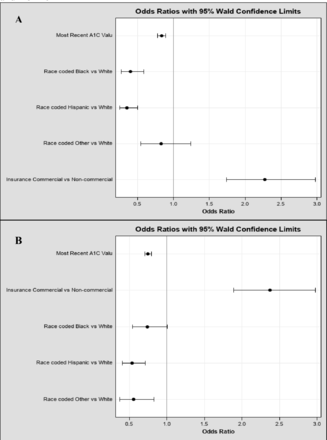
Results From August 2020 to 2021, independent of insurance payor status, non-Hispanic Black (NHB) and Hispanic youth with type 1 diabetes were less likely to use pump therapy (OR 0.4 and 0.35, respectively) or CGM (OR 0.74 and 0.54) compared with non-Hispanic White (NHW) youth. For pump eligibility, diabetes educators placed higher importance on subjective factors such as parental education, health literacy, and psychosocial stability (p value <0.05) compared with physicians. Hispanic and NHB patients and parents learned about diabetes technology later after diabetes diagnosis compared with NHW patients/caregivers. Physicians and diabetes educators, but not patients themselves, identified patient-perceived barriers to CGM use (ie, embarrassment and/or discomfort in wearing devices) as reasons for not utilizing diabetes technology.
Conclusions There are marked disparities in diabetes technology use among youth with diabetes. Findings from the provider surveys showed reliance on subjective variables as opposed to objective criteria. Youth with diabetes and caregivers of underrepresented race/ethnicities learned about diabetes technology later and were less likely to use technology. Though clinic providers perceived multiple barriers to technology utilization, responses from families showed low perceived burden and highly positive attitudes.
Introduction
There have been marked advances in diabetes care with the introduction of diabetes technologies such as insulin pumps and continuous glucose monitors (CGM). Compared with multiple daily injections or fixed insulin doses, insulin pumps, particularly the more advanced automated insulin delivery systems (AID), can lower hemoglobin A1c (HbA1c), improve metabolic variability, and decrease the incidence of both diabetic ketoacidosis and severe hypoglycemia.1 2 In addition, CGM use reduces HbA1c across all ages and insulin administration methods and reduces mild to moderate hypoglycemia.3 4 While technology use over the past few years has increased5 and the benefits are clear, there are persistent disparities nationwide in technology utilization.6 7 When controlling for gender, age, and diabetes duration, non-Hispanic White (NHW) children have the highest percentage of insulin pump use compared with non-Hispanic Black (NHB) and Hispanic children with type 1 diabetes (T1D).7 This disparity persists even when corrected for insurance type, household income, and parental education, suggesting the disparities are not only attributable to socioeconomic factors.7
The reasons for disparities in diabetes technology utilization are likely multifactorial and include provider and patient perceived barriers to technology uptake. Prior studies have shown provider-implicit bias pertaining to diabetes technology recommendations8 and different levels of clinician readiness in promoting newer diabetes technologies,9 which may unintentionally contribute to disparities. Medical providers are less likely to discuss potentially complex treatment plans with patients who they perceive to be less medically competent, and surveys of physicians indicate that these are often patients from historically marginalized communities.10 Another study showed that limited English proficiency (LEP) in parents predicts lower rates of diabetes technology utilization.11 Additionally, there may be personal (ie, single-parent household, older age at diagnosis), psychological (ie, depressive symptoms, diabetes distress), and structural (ie, insurance coverage, technology costs, lack of standardized patient education) factors that affect uptake and use of diabetes technology.12–15 The aim of this study was to assess racial, ethnic, and socioeconomic disparities in technology utilization and determine provider-, patient-, and caregiver-identified barriers to diabetes device adoption at a large urban pediatric hospital. We hypothesize that disparities in diabetes technology utilization will be present across race/ethnicity and primary language of caregiver but will not be related to health insurance coverage. Additionally, we expect that patients and caregivers from historically marginalized populations will have higher perceived burdens and lower expectations and negative attitudes about diabetes technology. Finally, we anticipate an alignment between patient/caregiver and clinician-perceived barriers to technology utilization.
Discussion
Our study of pediatric patients with T1DM found that Black and Hispanic patients were less likely to use diabetes technology such as insulin pumps and CGM even when adjusted for insurance status.6 7 These findings are consistent with other studies involving young patients and adults.6 7 23 Variability in timing when first learning about different forms of diabetes technology from their providers was consistent across patient and caregiver responses. Therefore, in addition to relying on objective criteria, as observed in the current study findings and previous reports,20 a clinical implication could be to implement a systematic and standardized approach to diabetes technology-related discussions and uptake. We learned that caregivers of patients who were not using CGM reported higher perceived burdens than CGM users, which may dissuade families from pursuing CGM for their children. One theory worth investigating in subsequent studies may be negative caregiver experiences with CGM in their own diabetes management.
NHB and Hispanic patients and caregivers had positive attitudes toward diabetes technology and positive expectations regarding AID use. This suggests that the trend of less technology utilization in historically marginalized populations is not due to disinterest in technology. Hispanic caregivers with LEP had higher perceived burdens to CGM compared with Hispanic English-speaking caregivers. Similarly, Hispanic patients had higher perceived burden to CGM use compared with NHW and NHB patients. Given that LEP caregivers of youth with complex medical conditions face many challenges in communicating with healthcare providers, it is likely that communication barriers play a significant role in accounting for this disparity.24 It is possible that clinicians have a lower inclination to offer insulin pumps to LEP families due to anticipated challenges in communication or a biased perception that they might not be good candidates for pump use. One qualitative study found that Spanish-speaking parents of children and adolescents with T1D cited reluctance to employ insulin pumps because of concerns that their child/adolescent would experience discomfort during sports or have less freedom in their dietary choices. The authors noted how these concerns were directly contradictory to the stated benefits of insulin pumps, suggesting possible miscommunication with medical providers or a general misunderstanding of the pump technology.25 This suggests an area of improvement to provide more culturally and linguistically appropriate resources for LEP families.
Limitations of this study include small sample sizes for caregivers with LEP. There may have been an element of recall bias, as participants were asked to think back to the time when they or their child was diagnosed with diabetes. Additionally, we are unable to measure the patient/caregiver knowledge of diabetes technology and were unable to assess whether discussions regarding diabetes technology were patient/family-initiated or provider-initiated. Race and ethnicity data were obtained from our electronic health record which may be discordant from how patients self-report their race/ethnicity. It is important to note that the goal of this study was to gain the perspectives of historically marginalized patients and the race/ethnicity demographics of the participants in this study are not representative of our clinic patient’s demographics.
Decisions to use diabetes technologies are multifactorial and influenced by provider prescribing practices, as well as patient and/or caregiver perceptions toward technologies. This study shows that clinic providers may place more importance on subjective factors rather than objective criteria, which is consistent with prior studies.20 Additionally, though clinic providers perceive many barriers to technology use by patients, the patient/caregiver responses suggest low burdens to certain forms of technology and overall positive attitudes.
The findings of our study provide an opportunity to increase awareness of potential bias and encourage providers to be more mindful of introducing diabetes technology to all patients using a standardized method. Future interventions could incorporate use of a shared decision-making model to allow for a systematic approach to discuss diabetes technology with patients and families.

Leave a Reply