Results
From the original cohort of 477 siblings in the HKFDS and 863 presumably unrelated individuals in the BHBHK, 583 individuals were included in the present analysis, of whom 235 individuals from 104 families had a FmH-YOD and 348 unrelated individuals reported no FmH of diabetes (FmH-NONE) (figure 1 and online supplemental figure 1). In this prospective cohort, 43.7% were men. The median age was 41 (36–47) years with a body mass index (BMI) of 23.3 (21.2–26) kg/m2, an FPG of 4.9 (4.6–5.2) mmol/L, 1-hour PG of 8.1 (6.4–10.1) mmol/L and 2-hour PG of 6.0 (4.9–7.3) mmol/L (table 1). Compared with the FmH-NONE group, the FmH-YOD group was younger (38 vs 44 years, p<0.001) and had higher BMI (23.8 vs 22.9 kg/m2, p=0.006), systolic blood pressure (120 vs 110 mm Hg, p<0.001), plasma triglycerides (1.1 vs 1 mmol/L, p=0.043), and a lower high-density lipoprotein-cholesterol (1.3 vs 1.6 mmol/L, p<0.001). The FmH-YOD group was more likely to smoke (15.5% vs 8.7%, p=0.011), have IFG (12.8% vs 6.6%, p=0.011), and IGT (27.2% vs 12.9%, p<0.001) than the FmH-NONE group (table 1).
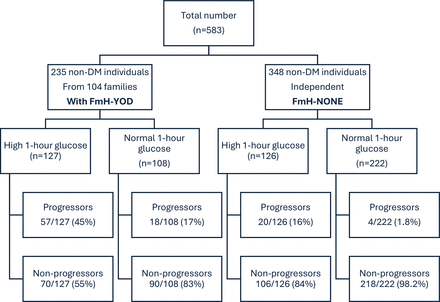
Overview of study participants stratified by FmH of diabetes and 1-hour plasma glucose during the 75-g oral glucose tolerance test at baseline. FmH, family history; YOD, young-onset type 2 diabetes; DM, diabetes mellitus.
•
Baseline characteristics of study participants by FmH of diabetes
At baseline, 54% in the FmH-YOD group had high 1-hour PG versus 36.1% in the FmH-NONE group (p<0.001). In the whole group, 40.3% and 19.8% of the high 1-hour PG group had concurrent IGT and IFG, respectively, with high 1-hour PG capturing most cases of IGT (93.6%) and IFG (94.3%) (online supplemental table 1). In the FmH-YOD group, 31.9% (75/235) developed diabetes compared with 6.9% (24/348) in the FmH-NONE group after a median follow-up of 12.1 (11.3–13.1) years. In the high 1-hour PG group, 45% (57/127) developed diabetes in FmH-YOD compared with 16% (20/126) in the FmH-NONE group. In the unadjusted model, FmH-YOD, 1-hour PG (centered at 4 mmol/L), and the interaction term (FmH-YOD×1-hour PG) had ORs of 20.2 (95% CI 5.3 to 77.6, p<0.001), 1.68 (95% CI 1.41 to 2.01, p<0.001), and 0.78 (95% CI 0.63 to 0.96, p=0.022), respectively, for incident diabetes (online supplemental table 3a). After adjusting for age, sex, BMI, and other cardiometabolic risk factors, including IFG and IGT, the ORs of FmH-YOD, 1-hour PG and (FmH-YOD×1-hour PG) for incident diabetes remained significant with respective values of 36.3 (95% CI 6.1 to 216.7, p<0.001), 1.48 (95% CI 1.16 to 1.88, p=0.002), and 0.72 (95% CI 0.55 to 0.93, p=0.013), respectively (online supplemental table 3b). The results remained similar when IFG and IGT were replaced with FPG and 2-hour PG as continuous covariates. We repeated the analysis by dichotomizing 1-hour PG with the cut-off at 8.6 mmol/L. After adjusting for the aforementioned confounders, including IFG and IGT, the negative association of (FmH-YOD×1-hour PG) with incident diabetes showed marginal significance (OR 0.211 (95% CI 0.037 to 1.20), p=0.079). Replacing IFG and IGT with FPG and 2-hour PG as covariates rendered the interactive term of (FmH-YOD×1-hour PG) nearly significant with an OR of 0.179 (95% CI 0.032 to 1.014, p=0.052) (online supplemental table 4).
To further examine this negative interaction between 1-hour PG and FmH-YOD, we classified participants into four groups: (1) FmH-NONE/normal 1-hour PG, (2) FmH-NONE/high 1-hour PG, (3) FmH-YOD/normal 1-hour PG, and (4) FmH-YOD/high 1-hour PG. After adjusting for confounders including IFG and IGT, (FmH-NONE/high 1-hour PG), (FmH-YOD/normal 1-hour PG), and (FmH-YOD and high 1-hour PG) groups had ORs of 7.4 (95% CI 1.6 to 35.1, p=0.011), 18 (95% CI 3.3 to 98.1, p=0.001), and 28.2 (95% CI 5.5 to 145.9, p<0.001), respectively, when compared with the (FmH-NONE/normal 1-hour PG) group (table 2).
•
Risk of incident diabetes at 2012–2014 follow-up, stratified by family history and 1-hour plasma glucose during 75-g oral glucose tolerance test at baseline
In ROC analysis, 1-hour PG predicted incident diabetes in both the FmH-YOD (area under ROC curve (AUROC) 0.688 (95% CI 0.616 to 0.760, p<0.001)) and FmH-NONE groups (0.829 (95% CI 0.758 to 0.899), p<0.001) with considerably lower performance in the FmH-YOD group (difference in AUROC (FmH-NONE–FmH-YOD)=0.141 (95% CI 0.040 to 0.241), p=0.006) (figure 2). In the FmH-NONE group, 1-hour PG had the highest AUROC (0.829 (95% CI 0.758 to 0.899), p<0.001) compared with FPG (AUROC 0.743 (95% CI 0.647 to 0.839), p<0.001) and 2-hour PG (0.783 (95% CI 0.688 to 0.877), p<0.001), although the differences were short of significance. In the FmH-YOD group, FPG had the highest AUROC (0.792 (95% CI 0.730 to 0.853), p<0.001) compared with 1-hour PG (AUROC 0.688 (95% CI 0.616 to 0.760), p<0.001) and 2-hour PG (AUROC 0.706 (95% CI 0.636 to 0.776), p<0.001). These differences in AUROC were significant (Difference in AUROC (FPG–1-hour PG) 0.104 (95% CI 0.033 to 0.174), p=0.004; Difference in AUROC (FPG–2-hour PG) 0.086 (95% CI 0.006 to 0.165), p=0.035). Among people with i-IFG (n=27), the conversion rate to diabetes was 66.7% in the FmH-YOD and 6.7% in the FmH-NONE group. We repeated the ROC analysis by randomly selecting one person from each family in the cohort, and the results remained similar and significant.
Out of the 583 participants included in the main analysis, 149 who were not defined to have diabetes at the 12-year follow-up based on electronic medical records did not have a complete set of OGTT (FPG, 2-hour PG) and HbA1c data for definite ascertainment of non-diabetes status at follow-up. As a sensitivity analysis, we excluded these 149 individuals and repeated the main analysis (n=434) including regression and ROC analysis, and the results remained similar and significant (all p<0.05 as in the main analysis [results not shown].
Receiver operator characteristics analysis of plasma glucose parameters during the 75-g oral glucose tolerance test for incident diabetes at the 2012–2014 follow-up. AUROC, area under receiver operator characteristics curve; FmH-NONE, no family history of diabetes; FmH-YOD, family history of young-onset type 2 diabetes; FPG, fasting plasma glucose.

Leave a Reply