Results
We analyzed data from 1220 adults with type 1 diabetes in France, covering 39 diabetic centers (online supplemental figure S3). The mean age was 42.0 (SD 13.9) years, with average diabetes duration at 24.7 (13.6) years, and 617 (50.6%) were females. Among SFDT1 respondents, 775 (63.5%) used insulin pumps, of which 150 (19.4%) used AID, 1145 (93.9%) employed CGM systems, and the mean HbA1c level was 7.6 (1.2)%. Participants who did not complete the PAID questionnaire (n=966) were predominantly male, younger, and had poorer glycemic control, and the majority were using MDI as their insulin treatment (online supplemental table S2).
The overall KMO index was 0.96, indicating very good suitability for EFA,36 which was used to identify DD subdimensions. Principal axis factoring with promax rotation extracted a six-factor solution, which explained 51% of the total variance (online supplemental table S3). The factors, representing DD subdimensions, were labeled following Dennick et al’s conceptualization study of DD11: emotional distress (α=0.90), fear of complications (α=0.73), social distress (α=0.78), eating distress (α=0.78), management distress (α=0.74), and diabetes burnout (α=0.86).
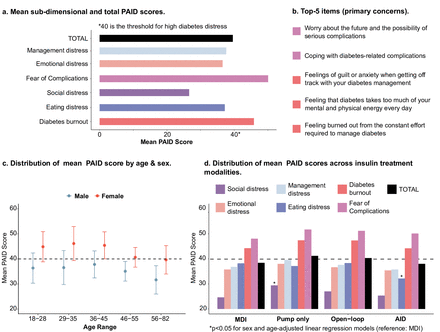
The mean PAID score was 39.6 (21.7), with the distribution of DD as follows: 213 participants (17.5%) in the low level, 415 (34%) in the moderate level, and 592 (48.5%) in the high level. The primary source of distress was fear of complications, as evidenced by a mean score of 50.1 (24.4) in this subdimension (table 1, figure 1a). Worrying about the future and serious complications (item 12) had the highest individual mean score (2.4 (1.1)), with 48.8% of participants considering it a somewhat serious (score 3) or serious problem (score 4). This item, together with feelings of guilt or anxiety about diabetes management (item 13) and coping with complications (item 19), constituted the top three items (figure 1b; top five are highlighted).
Problem Areas in Diabetes (PAID) characteristics in Suivi en France des personnes avec un Diabète de Type 1 (SFDT1). (a) Comparison of PAID scores by diabetes distress subdimensions. (b) Top five (ie, higher mean) PAID items. (c) Comparison of total PAID scores by age and sex. (d) Comparison of PAID scores across insulin treatment modalities. (c and d) Dashed lines at y=40 indicate threshold for high diabetes distress. AID, automated insulin delivery; MDI, multiple daily injections.
•
Clinical phenotyping of SFDT1 cohort: diabetes distress scores and individual and clinical characteristics of adults with type 1 diabetes and their associations with PAID levels
Tables 1 and 2 show the distribution of all explanatory variables across DD levels. Significant differences between moderate or high DD levels and the reference category, low DD, are highlighted in bold, with significance levels indicated by asterisks. The ORs and CIs from these associations are detailed in online supplemental tables S3 and S4.
•
Clinical phenotyping of the SFDT1 cohort: diabetes-related complications and psychological factors of adults with type 1 diabetes and their associations with PAID levels
Our analysis revealed that female sex and younger age were strongly linked to increased DD levels. This relationship is visually depicted in figure 1c; specifically, females were shown to have an average increase of 8.4 points in PAID scores compared with males.
Results from the age and sex-adjusted logistic regression models indicated that social vulnerability and current smoking were positively associated with high DD. Although clinical indicators did not reach statistical significance, there was a notable increase in HbA1c and GRI values from the low to high DD categories.
Our study found no association between PAID levels and diabetes duration, use of CGM or use of AID (table 1). Variations in DD between insulin treatment modalities were minor, with only a significant increase in social distress among insulin pump users and a reduction in eating distress among AID users, compared with the reference modality, MDI (figure 1d).
Among diabetes-related complications, only retinopathy was significantly associated with DD. Regarding psychological determinants, anxiety/depression, eating disorders, insulin misuse, impaired awareness of hypoglycemia, fear of hypoglycemia, treatment and glycemic burden were positively associated with high DD. Diabetes-dependent quality of life and sleep quality were negatively associated with DD.
A deeper examination of these associations indicated that psychological factors had the strongest association with DD (as shown by the highest ORs in figure 2 and detailed in online supplemental tables S4 and S5). Among individual characteristics, female sex showed the strongest association, followed by social vulnerability.
Clinical phenotyping of Suivi en France des personnes avec un Diabète de Type 1 (SFDT1) cohort participants: significant associations (p<0.05) between study variables and moderate (circle) and high (triangle) diabetes distress levels (reference: low). Red: positive association (OR>1). Blue: negative association (OR<1). The lines represent ORs and 95% CIs from age and sex-adjusted multivariable logistic regression models. Age and sex variables are adjusted for each other. DD, diabetes-related distress; QoL, quality of life.

Leave a Reply