Introduction
People living with obesity face negative attitudes, stereotypes, and blame from others because of their weight (ie, weight bias).1 Weight bias can be explicit, such that an individual is conscious of negative attitudes (ie, blatant), or it can be implicit, where the person is unwilling or unable to admit these attitudes (ie, unconscious).2 Weight bias is partly driven by the inaccurate belief that weight is entirely within an individual’s control.3 This conceptualization ignores the complex genetic, biological, social, financial, environmental, and behavioral factors contributing to obesity. This complexity contributes to the challenge of losing weight and maintaining a lower body weight, especially through self-directed nutritional changes and exercise alone.
Weight bias leads to weight stigma, or the social devaluation and mistreatment of individuals based on weight or size.4 Examples of weight stigma include the perpetuation of negative weight stereotypes in media outlets; weight-discriminatory policies and practices (including in healthcare settings); discrimination in employment and education; and teasing, bullying, harassment, or other subtler instances of interpersonal rejection, avoidance, or criticism.5 Even without direct experiences of weight stigma, many individuals come to anticipate negative judgment or mistreatment from others because of their weight.6 Notably, some people living with obesity internalize stigma by absorbing negative weight attitudes and stereotypes—and ultimately devalue themselves because of their weight (ie, self-stigma).7
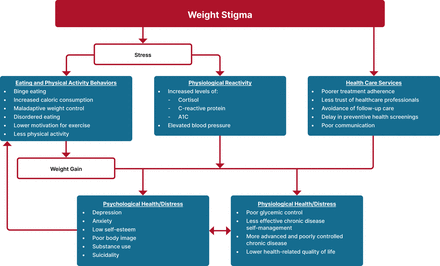
Weight stigma is consistently and robustly linked to adverse physical and mental health outcomes8–11 (figure 1). Weight bias and stigma lead to lower healthcare quality and contribute to individuals with obesity having reduced access to and utilization of healthcare services. Weight bias has been documented in healthcare professionals across specialties,12 and weight stigma occurs at multiple levels in the healthcare setting,13 including structural or institutional stigma (eg, in healthcare policies or clinic environments), interpersonal stigma (eg, in interactions with healthcare professionals), and intrapersonal stigma (within individuals with obesity). Examples of weight stigma in healthcare settings include denial of care to individuals with obesity (eg, due to body mass index cut-offs), disrespectful or dismissive communications, and assumptions that all health problems are attributable to weight14 (figure 2). Healthcare professionals must actively work to prevent and reduce weight bias and stigma to improve care and enhance health.
Health consequences resulting from experiences of weight stigma (adapted from Puhl et al [11]).
Examples of weight bias and stigma at multiple levels. Weight bias and stigma can occur at multiple levels within the healthcare setting, contributing to reduced quality, accessibility, and utilization of healthcare services.
The methodology and procedures for this section of Standards of Care in Overweight and Obesity focus on evidence-based clinical recommendations to assist healthcare professionals, researchers, and people living with obesity in managing overweight and obesity. These guidelines are developed by the Professional Practice Committee (PPC) of the American Diabetes Association (ADA)’s Obesity Association, an interprofessional team of experts in fields such as obesity medicine, endocrinology, behavioral health, and public health. Additionally, several obesity organizations, including the American Board of Obesity Medicine Foundation (ABOMF), American Society for Metabolic and Bariatric Surgery (ASMBS), Obesity Action Coalition (OAC), Obesity Medicine Association (OMA), and The Obesity Society (TOS), are represented on the Standards of Care through the inclusion of society members in the PPC. Appointments to the PPC consider clinical and research excellence and ensure diverse representation. Subcommittees conduct systematic literature reviews to inform updates, guided by a methodologist and librarian. Recommendations are graded based on evidence quality (A, B, C, or expert opinion E), with the strongest evidence derived from large, well-designed randomized clinical trials. While evidence forms the basis, recommendations prioritize individual personal needs and preferences, emphasizing nuanced, person-centered care. For full details, please see the Introduction and Methods section.
The development process ensures transparency, requiring all contributors to disclose potential conflicts of interest, which are rigorously reviewed. No pharmaceutical or medical device companies fund the guideline, and contributors receive no remuneration. Recommendations are deliberated on by PPC members, with an 80% consensus required for approval. The guideline undergoes annual updates to reflect evolving evidence, supplemented by public comments to address care gaps and improve transparency. External peer reviews and adherence to established guideline development principles ensure credibility and rigor in this comprehensive approach to optimizing care for individuals with overweight or obesity.
In alignment with the Lancet Commission on Obesity, the ADA’s Obesity Association recognizes the importance of acknowledging and addressing weight bias and stigma to provide the most optimal care to individuals with obesity.15 The ADA’s Obesity Association has developed comprehensive guidelines to address weight bias in healthcare, recognizing it as a significant barrier to effective obesity management. These guidelines focus on three critical areas: education and training, clinical environment and practice, and communication and collaboration. Each area is crucial in fostering an inclusive healthcare system that provides equitable and compassionate care for individuals with obesity.
Recommendation
1.1 All clinicians and staff should be trained on weight bias and stigma. [C]
Healthcare professionals receive minimal education and training on obesity,16 which may contribute to a misinformed workforce that unfairly assigns blame and negative stereotypes to individuals with obesity. Implicit and explicit weight bias has been consistently observed among trainees in medicine and other healthcare disciplines.17–22 Given this evidence, education on weight bias and stigma should begin early in training for healthcare professionals, including prehealth and premedical undergraduate students, medical and other graduate students in health-related fields, residents, fellows, and other trainees. Weight bias persists throughout and beyond medical training,12 17 23 24 and weight bias intervention effects diminish over time,25 so continued education is needed for practicing clinicians.
A recent meta-analysis and several systematic reviews have examined the effects of education and training interventions to reduce weight bias among healthcare professionals.25–27 Results showed small-to-moderate effects of interventions on weight bias, with moderate-to-substantial heterogeneity.26 Comparisons of effects between different types of interventions have not been conducted. Therefore, until more data become available, training approaches and modalities described here are considered acceptable to use. Research on this topic has focused on training for clinicians, but it is also recommended that support staff receive appropriate training. The purpose of weight bias training is to improve care for people living with overweight and obesity. However, these trainings would likely also benefit any employees with overweight or obesity by contributing to a more weight-inclusive clinical/workplace culture.28
Studies have primarily tested the short-term effects of training interventions on explicit weight bias among students, with less research focused on practicing clinicians, implicit bias, or long-term effects. Training modalities include lectures, videos, clinical vignettes, role-plays, simulations, reflective journal exercises, interactive discussions, or combinations of multiple modalities. Some training courses are conducted over multiple sessions, while others are provided as a single workshop. Training approaches predominantly target beliefs about the causes of obesity and its controllability to reduce blame, mainly through providing basic education on obesity and weight bias.25 26 This approach emphasizes recognizing the complex interactions among genetic, biological, behavioral, social, and environmental factors that affect weight and weight management (rather than an oversimplified view of obesity as caused solely by low-quality nutrition and sedentary behavior). Other training approaches focus on evoking empathy (eg, by engaging with individuals who have lived experiences of weight stigma), increasing self-awareness of bias (eg, through reflective journaling or completing the Implicit Association Test),29 enhancing weight-related counseling skills (eg, through interactions with clinical actors), emphasizing a weight-neutral approach to care, and changing social norms through tactics such as role-modeling and role-playing.25 27
In a study of 127 first-year medical students, participants read short articles about weight bias and weight-related communication strategies before completing a simulation exercise to discuss weight with clinical actors who identified as having overweight or obesity.30 Afterwards, the clinical actors and their peers provided participants feedback and attended an additional discussion session to engage in further self-reflection. Results showed significant reductions in weight-based stereotyping and significant increases in empathy and confidence in clinical interactions with individuals with obesity; the latter two improvements were sustained at 1 year follow-up. In another study of 67 kinesiology undergraduate students,31 blame towards individuals with obesity significantly decreased among participants who received an intervention that included a lecture about the uncontrollable causes of obesity and weight bias, brief videos about the complex etiology of obesity, and a role-play exercise to practice communicating with individuals about weight (compared with a control group that received a more traditional lecture and video content about controllable causes of obesity, such as nutrition and exercise). Notably, results did not show improvements for other facets of explicit bias (stereotypes and perceived attractiveness) or implicit bias.
Research on implicit bias training for healthcare professionals is generally lacking across all forms of implicit bias,32 and some unintended consequences of such training (such as psychological reactance) have been documented.33 Still, current evidence suggests that several strategies can potentially reduce implicit bias and its negative consequences, including structured, curriculum-based education, engaging in positive interactions with stigmatized individuals, role-modeling, and changes to the climate or culture within a healthcare setting or training environment.32 Training should go beyond a sole focus on attitudes by introducing concrete behavioral strategies that can mitigate the effects of implicit bias on care for individuals with obesity, ideally with multiple training sessions to allow time to practice these strategies.32 34
Multicomponent training is likely to yield more benefits than single-component interventions and is recommended when feasible to reduce implicit and explicit weight bias and subsequent harms. In particular, training including both foundational education and active or hands-on learning may be most effective.34 For example, a recent study tested the effects of a 4-hour virtual continuing medical education (CME) symposium that included the following intervention components: didactic lectures that emphasized uncontrollable contributors to obesity (to reduce blame); a panel of individuals with obesity that discussed experiences of weight stigma (to increase empathy); completion and discussion of results from the Implicit Association Test (to raise self-awareness of bias); and signing a pledge to contribute to the reduction of weight bias in healthcare (to create a culture that discourages weight bias and stigma).35 The CME course was completed by 218 healthcare professionals within a health system. Results showed significant reductions in weight bias and significant increases in empathy and confidence in treating individuals with obesity. In addition, compared with a control group of healthcare professionals who did not complete the training, participants who completed the CME course were more likely to diagnose obesity and refer individuals to obesity treatment 12 months later. This preliminary evidence suggests that providing multicomponent weight bias training can potentially reduce weight bias and positively affect the treatment of obesity.
Several types of resources are available to aid in training healthcare professionals (table 1). Healthcare systems, departments, or clinics can train their clinicians and staff internally, or they may refer clinicians and staff to external resources. Training clinicians and staff to follow the specific behavioral recommendations in these professional practice guidelines is also intended to reduce weight bias and stigma.
•
Weight bias and stigma training resources for healthcare professionals and individuals with obesity
Recommendations
1.2 Implement protocols to minimize risk of stigmatization during provision of healthcare services, including anthropometric measurements and communication practices for person-centered care. [E]
1.3 Ensure availability of clinical equipment and furniture that accommodates all individuals (eg, waiting room chairs, examination tables, gowns, blood pressure cuffs, high-capacity scales). [C]
1.4 Make accommodations to provide privacy during anthropometric measurements, including locating the scale in a private area. [E]
The clinical practice environment may include sources of stigmatization for people living with obesity, and these triggers within the clinical environment contribute to healthcare avoidance and delays.36–38 Given the risk of weight stigmatization in healthcare settings, clinical practices should consider modifications to ensure that all individuals feel welcome in the healthcare environment. Prior research has demonstrated that the lack of appropriate medical equipment contributes to perceptions of weight stigma and healthcare avoidance by people living with obesity.37 39 40 Box 1 provides a brief Clinical Practice Checklist of examples of recommended modifications for all clinical practices.41–43 Studies have shown that an inclusive clinical setting can lead to better health outcomes and increased satisfaction for individuals with obesity.44 Additional detailed clinical practice checklists are available online from the University of Connecticut42 and Obesity Canada.43 Research has found that clinics commonly lack items to accommodate individuals with obesity, particularly extra‐large blood pressure cuffs and gowns and adequate chairs in the waiting area.41 In addition, few practices have wheelchair-accessible scales and height-adjustable examination tables.45
Clinical practice checklist—minimum accommodations
Waiting Room
-
Sturdy chairs with double-width seats (35 in) or firm loveseats with weight capacity ≥300 lbs (136 kg)
-
Ensure 6–8 inches of space between chairs
-
Weight-sensitive media including reading materials, artwork, video displays
-
Available bariatric wheelchairs with extra-wide seat and weight capacity ≥300 lbs (136 kg)
Exam rooms
-
Sturdy chair with weight capacity ≥300 lbs (136 kg) and double-width seat (35 in)
-
Wide examination table with weight capacity ≥500 lbs (227 kg)
-
Large, extra-large, 2XL and 4XL size gowns
-
Large and extra-large adult and thigh blood pressure cuffs
As the waiting room is an individual’s first experience with the clinic, modifications to furniture and media in this area are key to establishing a welcoming environment.46 The waiting room should include double-width chairs with and without arms with a weight capacity of at least 300 lbs (136 kg) and ideally 700 lbs (315 kg) for practices focusing on obesity care.41 43 In addition, reading materials, posters, artwork, and video displays should avoid images or content stigmatizing individuals with obesity.41 43
Clinics should design and implement protocols for the performance of anthropometric measurements that include best practices for measurement, necessity for privacy, and communication of this information to the individuals under their care. Accommodations should be made to ensure privacy during weighing and other anthropometric measurements, such as placing the scale in a private location.41–43 Attention to individuals’ experience during weight measurement is particularly important, as this activity is often cited as a source of stigmatization for people living with obesity.38 47 Measurements should be performed and reported non-judgmentally. If the individual declines weight measurement, the healthcare professional should consider possible prior stigmatizing experiences and query for concerns. The scale should have a wide platform with supportive handles, be wheelchair-accessible, and have a weight capacity of at least 500 lbs (227 kg), but ideally 800 lbs (360 kg) for practices focusing on obesity care.41 43 The Agency for Healthcare Research and Quality (AHRQ) National Center for Excellence in Primary Care Research on Integrating Primary Care Practices and Community-based Resources to Manage Obesity includes resources that may assist with protocol and quality improvement initiatives for obesity.48
Exam rooms should be assessed to ensure that the furniture and equipment accommodate all individuals. The examination table should be wide with a weight capacity of at least 500 lbs (227 kg), but ideally 800 lbs (360 kg) for practices focusing on obesity care.41 43 If possible, an examination table with electric lift and hydraulic tilt features should be used to enable height adjustment of the table to facilitate transfers of individuals with obesity. If these features are unavailable, the clinic should provide a step stool with a handle to assist with exam table access. Clinics may consider bolting exam tables to the floor to increase stability. All clinics should have multiple gown sizes that include gowns at least 4XL in size. Sphygmomanometers should be selected to accommodate extra-large adult and thigh blood pressure cuffs, and these cuff sizes should be available in all exam rooms and measurement locations. Clinical practices that provide gynecologic or obstetric care should have vaginal speculae in a variety of sizes as well as both plastic and metal versions available. Clinics who lack proper speculae contribute to weight stigmatization.37 Clinicians should also be aware of phlebotomy and imaging centers, which have the necessary equipment to accommodate individuals with obesity.
When possible, the clinic’s physical space or floor plan should accommodate individuals living with obesity.41 46 49 Doors and hallways should accommodate large-size mobility equipment such as wheelchairs, walkers, and scooters. If elevators are present, their weight capacity should be at least 700 lbs (315 kg) and be able to fit a bariatric wheelchair. Bathrooms should have properly mounted grab bars and floor-mounted toilets, and the room should be sized to allow for large-size mobility equipment. A wall-mounted sink is also recommended. A split lavatory seat with handled urine specimen collector should be installed when relevant to the clinical practice.
Recommendations
1.5 Use person-centered, nonjudgmental language that fosters collaboration between individuals and healthcare professionals, including person-first language (eg, “person with obesity” rather than “obese person”). [E]
1.6 Engage individuals in shared decision-making to individualize diagnostic and treatment approaches, including collaborative goal setting beyond weight reduction. [C] Support and collaborate with individuals on long-term obesity care. [C]
1.7 Ask permission to discuss weight with individuals. If individuals decline, respect autonomy and refrain from forcing conversation. If individuals accept, inquire about their preferred terms/words to discuss weight. [C]
Obesity is a complex and often sensitive topic, making communication about obesity challenging for both healthcare professionals and individuals with obesity. Bias and stigma around weight and obesity may leave individuals feeling shamed or judged by healthcare professionals,50 which may contribute to feeling reluctant to discuss weight loss or obesity—or even avoid healthcare interactions entirely.
The terminology used in clinical settings may introduce or mitigate weight bias and perceived stigma in conversations with healthcare professionals. Table 2 provides examples of preferred language, both verbal and written. The use of person-centered language (eg, ‘person with obesity’ is preferred over ‘obese person’) is strongly encouraged to support productive clinical interactions. Multiple scientific journals prohibit submissions with pejorative language that describes persons with obesity or writing that attributes moral judgments or character flaws to people living with obesity,51 52 emphasizing the need for respectful and person-first language in clinical practice and research. Person-centered language recognizes a medical condition rather than implying judgment about the individual.53 Avoid using the term ‘obese’, as well as pejorative-sounding adjectives such as ‘morbid’, ‘super’, or ‘extreme’, which are often used to describe the severity of obesity. Instead, obesity should be referenced using stages of severity (I, II, III).54 One practical tip around language is to ask individuals what terms they prefer to use when discussing their obesity or body weight. Other terms that might contribute to bias and stigma include language that appears to assign blame. Instead, it is recommended55 to use objective terms such as ‘sub-optimal clinical response’ instead of ‘failure’, ‘recurrence’ instead of ‘recidivism’, and ‘barriers to adherence’ instead of ‘non-compliance’.56 Finally, clinicians should consider modifying the diagnostic codes used for billing, as several codes contain stigmatizing language, and many individuals can now view these codes in their medical records. In 2024, several new diagnosis codes for obesity were launched that avoid stigmatizing terms and enable a description of obesity severity (eg, E66.813 — Class 3 Obesity).
•
Examples of preferred language
In addition to language, it’s important to remember that not all individuals with obesity wish to receive obesity care.57 As such, healthcare professionals should ask permission to discuss obesity/weight and only proceed if permission is granted.58 59 If an individual does not grant permission, healthcare professionals are encouraged to focus on other health issues, leaving the option to focus on weight/obesity in the future when the individual is ready.
Shared decision-making (SDM) for obesity relies on a healthcare professional and an individual living with obesity working together to develop a specific obesity care plan that considers the individual’s health and preferences, values, and goals.60 61 SDM between individuals and professionals improves health outcomes and improves engagement.62 For obesity care, SDM includes the professionals presenting a range of obesity treatment options, including behavioral, medical, and surgical interventions, as appropriate, alongside discussions of the risks and benefits of each. It is important to remember that everyone may have different goals for their obesity care, and these can differ from their clinician’s goals. For example, an individual’s goal might be having the functional ability to get on the ground to play with their children versus a healthcare professional with more cardiometabolic-focused outcomes.
Identifying qualitative goals through SDM signals to the individual that the healthcare professional values personalized goals beyond weight loss. Goal setting can further enhance the partnership and contribute to long-term success, which is not only defined by total weight lost. Recognizing an individual’s qualitative goals, sometimes referred to as ‘non-scale victories’, can also help the individual feel valued by the healthcare professional and let them know that the clinician is invested in their overall health and well-being.

Leave a Reply